Evaluation of Virtual Wards in Greater Manchester
What did we do?
We undertook an independent evaluation of the Virtual Wards service being implemented across Greater Manchester (where it is known as Hospital at Home). We aimed to:
- Understand how Hospital at Home is organised and delivered across GM
- Explore patient, carer, and staff experiences of receiving or providing care by Hospital at Home
- Assess whether Hospital at Home provides an efficient and equitable approach to delivering care
Why was it important?
The health and care system across England was challenged with implementing a Virtual Wards service by December 2023.
The British Geriatrics Society definition of a Virtual Ward is
“a time-limited service enabling people who have an acute condition or exacerbation of a chronic condition requiring hospital-level care to receive this care in the place they call home, either as an alternative to hospital admission or by facilitating an earlier discharge from hospital.”
NHS England describes Virtual Wards as
“allowing patients to get the care they need at home safely and conveniently, rather than being in hospital” (see here for more information).
Crucially, Virtual Wards deliver a variable combination of remote monitoring and face-to-face treatment in the person’s normal place of residence (at home or in a care home). Implementation of Virtual Wards, supported by NHS England funding via Integrated Care Systems, includes an element of technology to help staff to monitor patient physiological observations remotely.
ARC-GM researchers Prof. Emma Vardy and Dr Gill Norman co-authored a Position Statement published by the British Geriatrics Society (BGS) about Virtual Wards in relation to older people.
A rapid evidence synthesis (RES) by ARC-GM published in Age & Ageing indicated the limited evidence available in relation to clinical effectiveness of Virtual Wards. Importantly the publication described a practical synopsis of terminology used in clinical practice in relation to Virtual Wards, hospital at home and remote monitoring.
Our evaluation of Virtual Wards in Greater Manchester offered us an opportunity to work closely with our key stakeholders to inform regional and national decision-making about this new way of working.
Prior to this study, ARC-GM researchers undertook a systematic review of technology-enabled innovations of Virtual Wards and hospital at home. The analyses, which included 69 studies (38 randomised and 31 non-randomised) and described 63 interventions, found that none of the technology-enabled care at home models explored put people at higher risk of readmission compared with hospital-based care. There also appeared to be no additional risk of mortality due to use of technology-enabled at home models. It was unclear whether inpatient-level care at home using higher levels of technology provided additional benefits.
How did we do it?
We used a mixed-methods approach to address priority questions identified by key GM stakeholders. The broad areas of interest included:
- Implementation and delivery of the Virtual Wards service
- Referral and admissions processes
- Organisation of care
- Experiences of patients and carers in receipt of the service
- Experiences of staff providing the service
In addition to system stakeholders, we involved members of the public in co-producing our research questions. At the start of the project, public members were consulted on what the broad areas of focus should be.
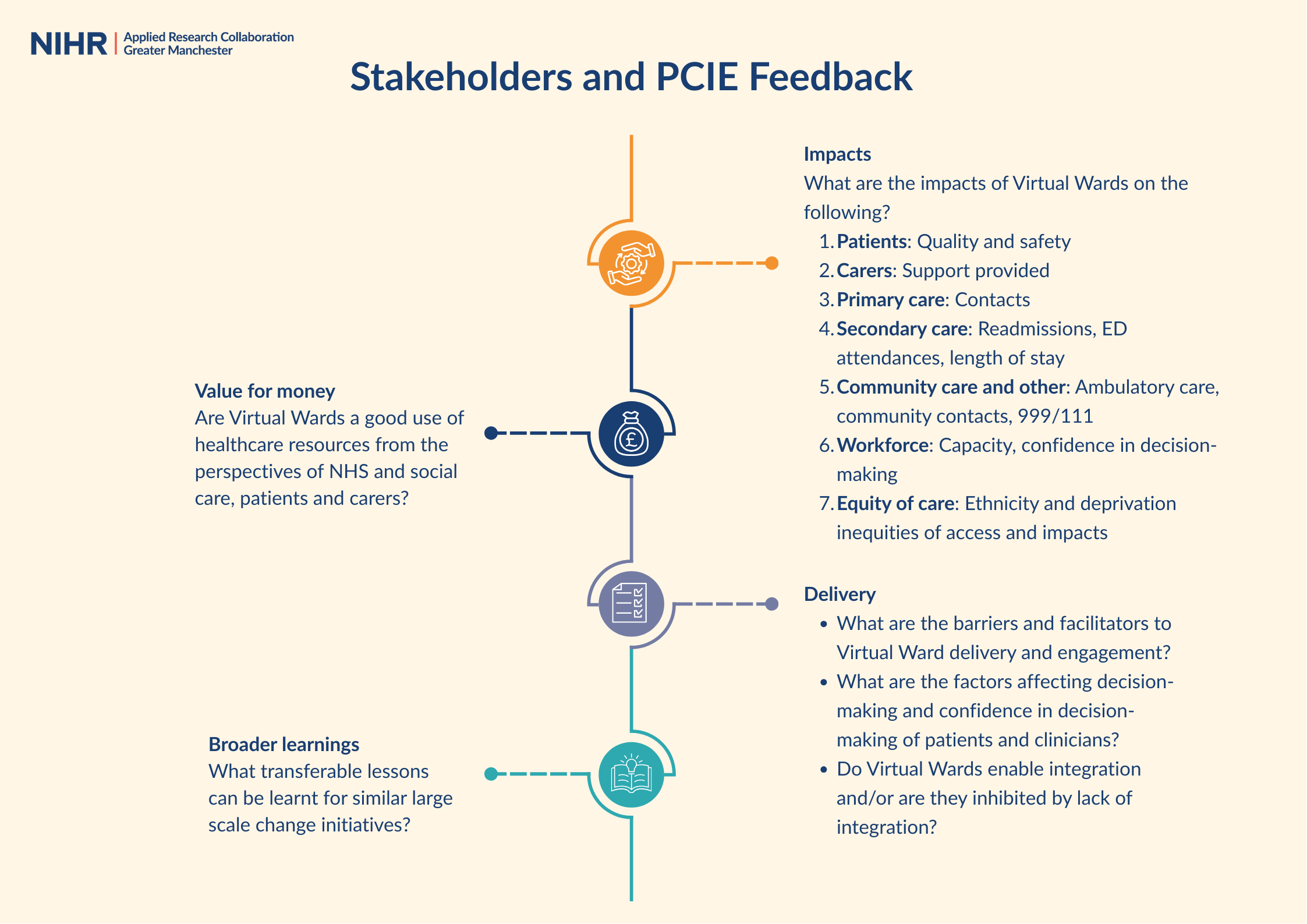
The study consisted of three key work packages:
Work Package 1: Understanding how Virtual Wards are being implemented and delivered in GM
This package involved:
- Qualitative interviews with Virtual Ward service and implementation leads to explore topics such as the key components of the Virtual Wards models adopted, how the Virtual Wards service is integrated at the system level, and the processes for referral, eligibility assessment, and admission
- Analysis of Virtual Wards data held by the NHS to understand the extent of Virtual Wards activity generated across GM, how it has changed over time, and to inform qualitative interviews. This included summarising Virtual Wards capacity and activity by locality, day of the week, care pathway, step-up versus step-down models of care, and patient demographics
Work Package 2: Understanding patient, carer, and staff experiences of receiving and providing care on Virtual Wards in GM
We collected in-depth qualitative data from four NHS case study sites to explore:
- Staff, patient, and carer experiences through interviews
- How different patients and providers experience Virtual Wards and what being on a Virtual Ward is like through observations in Virtual Ward settings and patients’ homes
Work Package 3: Assessing clinical, cost and system outcomes of Virtual Wards in GM
We assessed the outcomes of Virtual Wards using quantitative data for all 10 GM boroughs, focusing on:
- Assessment of cost
- Impact of the Virtual Wards care model on system-level healthcare utilisation and waiting times
Use of the Greater Manchester Secure Data Environment
Public and Community Involvement and Engagement
We collaborated with the ARC-GM PCIE Theme, the NIHR Greater Manchester Patient Safety Research Collaboration (PSRC) and Made by Mortals to continue our public involvement work throughout the project, ensuring that we heard the voice of people who might use the service. Members of the ARC-GM PCIE Panel and wider community groups were key to producing public-facing material which explores some of these insights.
Who did we work with?
- Health Innovation Manchester
- The Greater Manchester Virtual Ward Programme Board, part of the Greater Manchester Integrated Care Partnership (NHS Greater Manchester)
- NIHR Greater Manchester PSRC
- NIHR ARC Yorkshire & Humber
- NIHR GM PSRC - Engagement work website
- Publications
- Shi C, Dumville J, Rubinstein F, Norman G, Ullah A, Bashir S, Bower P & Vardy E R L C. (2024) Inpatient-level care at home delivered by virtual wards and hospital at home: a systematic review and meta-analysis of complex interventions and their components. BMC Medicine.
- Norman G, Bennett P, Vardy E, (2023). Virtual wards: a rapid evidence synthesis and implications for the care of older people, Age and Ageing, Volume 52, Issue 1, January 2023, afac319
- Norman, G. (2023). Rapid Evidence Synthesis: Virtual Wards (hospital at home) for Acute Admissions.
- Guidelines
- News Stories
- Blogs
- Using Rapid Evidence Synthesis to mobilise innovation in a rapidly changing NHS landscape by Dr Paula Bennett
- Sharing virtual wards RES evidence base to influence system-wide change by Prof Emma Vardy
- Virtual Wards RES shows value of evidence synthesis for large scale transformation programmes by Dr Gill Norman
- Podcasts
- Conferences
Contact information:

Programme Manager
Dr Ross Atkinson
ross.atkinson@manchester.ac.uk