DIPLOMA – Evaluation of the national NHS Diabetes Prevention Programme
Diabetes Prevention – Long term Multimethod Assessment (DIPLOMA) of the implementation, delivery and outcomes of the ‘Healthier You: National Health Service Diabetes Prevention Programme’ (NHS DPP)
What is the Diabetes Prevention Programme?
In 2015, NHS England; Public Health England; and Diabetes UK initiated a nationwide pilot of a Type 2 Diabetes Mellitus (T2DM) prevention programmem; consisting of seven demonstrator sites, including one in Salford. The demonstrator sites were used to test new novel approaches to identify patients who had a higher risk of developing T2DM, to help define and shape the roll-out of a national programme.
The NHS Diabetes Prevention Programme (NHS DPP) was rolled out in 2016 in England. Delivery was commissioned to four private provider organisations - Ingeus UK , Reed Momenta, ICS Health & Wellbeing and Living Well Taking Control.
The first wave covered 26 million people, half the country population, providing lifestyle advice to reduce participants’ risk of developing Type 2 Diabetes. By August 2018 the NHS DPP had been rolled out across all England. In 2019, the NHS Long Term Plan doubled funding for the NHS DPP, increasing capacity from 100,000 to 200,000 places per year by 2023. Having piloted a Digital DPP delivery throughout 2018, in 2019 the NHS DPP introduced a new framework which included a digital programme in addition to the initial face to face programme, this with the aim to increase programme reach.
Why is it important?
The increasing number of people being diagnosed with T2DM and at risk of complications has made the disease a major public health concern. Being diagnosed with NDH can provide an early warning that people are at risk of developing T2DM. Blood glucose levels, along with associated risks of developing T2DM, can be reduced by addressing lifestyle choices.
The NHS DPP is a publicly funded programme. It is the first T2DM prevention intervention delivered at national scale, providing lifestyle behaviour change education with the aim to reduce the major public health risk that T2DM is. Hence it is important to have an independent evaluation of the NHS DPP to assess:
- whether the programme is accessing the patient populations at greatest risk,
- whether patients receive a high-quality diabetes prevention course from their local provider,
- if the programme is delivering value for money, and
- to advise what could be done to achieve long-term sustainability nationwide.
How did we do it?
DIPLOMA – Evaluation of the NHS DPP was commissioned by the National Institute of Health Research (HS&DR 16/48/07). Initially, DIPLOMA was funded to evaluate NHS DPP’s Framework 1. Following the introduction of a digital intervention in Framework 2, DIPLOMA received funder approval to extend its scope to include assessment of the digital elements.
DIPLOMA was a comprehensive programme of work, led by researchers from The University of Manchester and University College London. It comprised of nine distinct but complimentary work packages, which made use of both quantitative and qualitative methods to assess the following:
- Access and equality - whether the programme provides fair access for all patients;
- Implementation - exploring how implementation differs across the country;
- Service delivery and fidelity - checking what is being delivered and how it compares to expectations;
- Patient decision-making and their experience;
- Outcomes and variation - assessing outcomes for patients engaged in the programme;
- Comparison of uptake and outcomes between the face-to-face DPP and digital DPP;
- Comparative effectiveness - analysing the programme vs. routine care in preventing T2DM;
- Validation study - a study to collect data on the potential barriers to access;
- Comparative long-term cost-effectiveness - to assess whether the NHS DPP is cost-effective compared to usual care in terms of long-term costs and benefits.
To read our fair processing statement, click here.
The study finished in March 2023 and a final report has been provided to the funder. However as research findings emerged from this national evaluation, we have provided feedback to NHS DPP stakeholders to support the ongoing development of the NHS DPP Programme. All of the findings from indivudaul workpackages have been published with open-access in peer-reviewed journals.
Findings
Behaviour Change Video: Our DIPLOMA Patient and Public Involvement group co-produced this video on behaviour change, summarising the types of behaviour change activities people might be encouraged to try when they join a programme such as the NHS Diabetes Prevention Programme.
(published May 2023)
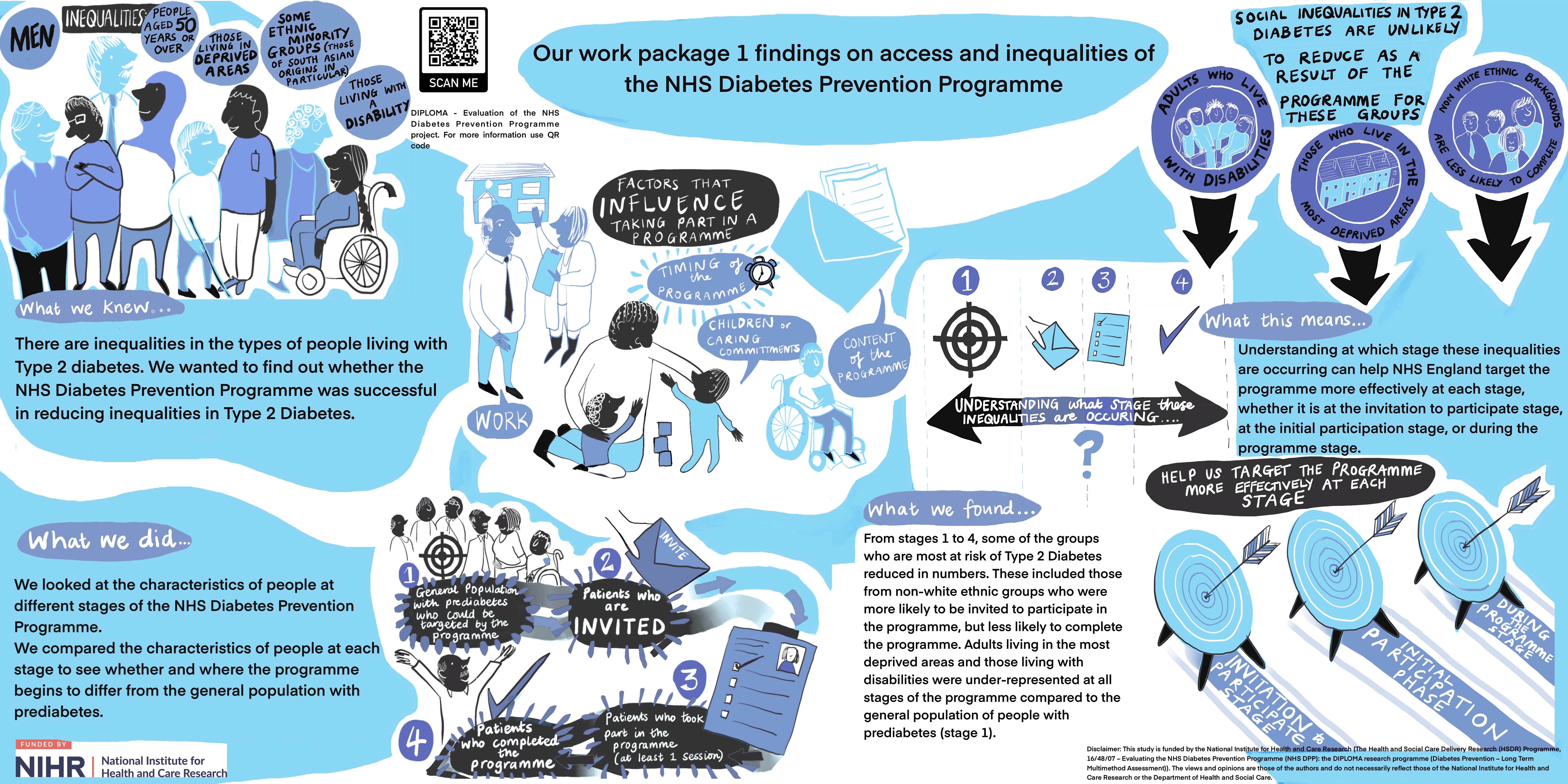
Our work package 1 findings on access and inequalities of the NHS Diabetes Prevention Programme
(click the image to enlarge)
Findings from the evaluation of the NHS Digital Diabetes Prevention Programme
(published March 2023)
Findings from the evaluation of Healthier You: The NHS Diabetes Prevention Programme
(published June 2022)
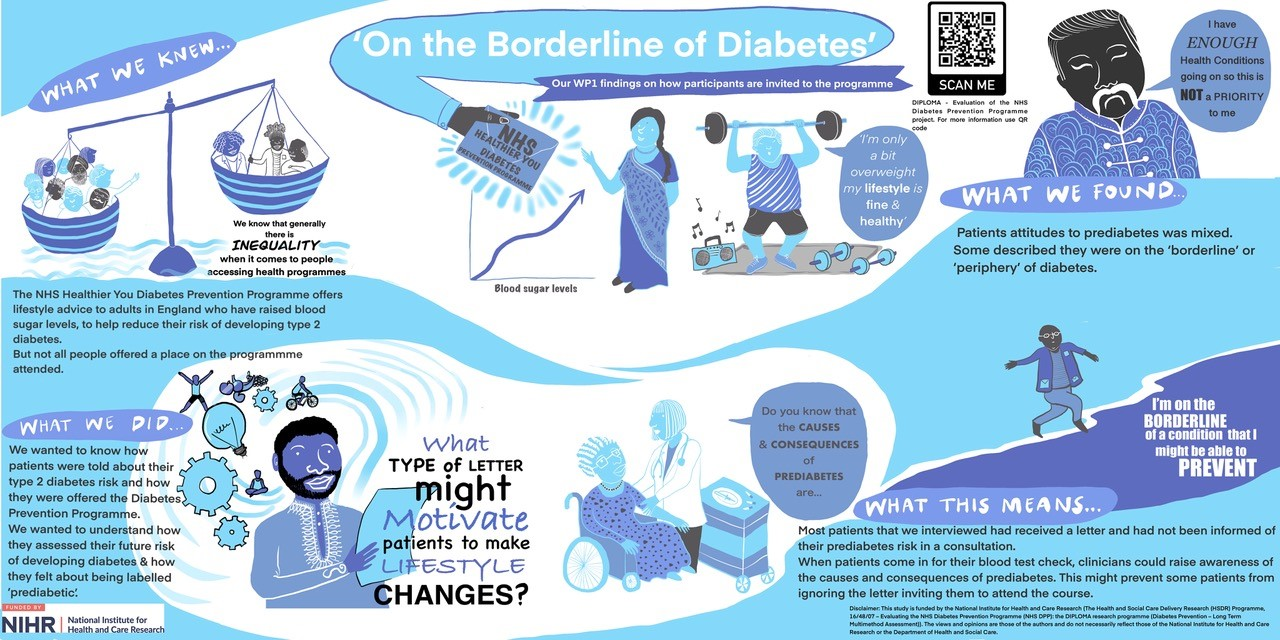
On the boader line of diabetes: findings on how participants were invited onto the NHS Healthier You Programme
(click the image to enlarge)
Taking steps towards preventing diabetes: Our findings on access to the NHS Healthier You Programme
(published November 2021)
Planning for Prevention
Visit the Policy@Manchester Planning for Prevention report where you can read more about:
- what was learnt from the Diabetes Prevention Programme and
- the Health Prevention Programmes
Who we worked with?
- NHS England
- Public Health England
- Diabetes UK
- National Institue of Health Research (NIHR)
- University of Sheffield
- University Collage London
- Publications
- Ross J, Hawkes RE, Miles LM, Cotterill S, Bower P, Murray E. (2023). Design and Early Use of the Nationally Implemented Healthier You National Health Service Digital Diabetes Prevention Programme: Mixed Methods Study. Journal of Medical Internet Research
- Hawkes R, Miles L, Ainsworth B, Ross J, Meacock R, French D. (2023). Engagement with a nationally-implemented digital behaviour change intervention: Usage patterns over the 9-month duration of the National Health Service Digital Diabetes Prevention Programme. Internet Interventions.
- Hawkes R E, Sanders C, Soiland-Reyes C, Brunton L, Howells K, Bennett C, Lowndes E, Mistry M, Wallworth H & Bower P. (2023). Reflections of patient and public involvement from a commissioned research project evaluating a nationally implemented NHS programme focused on diabetes prevention. Research Involvement and Engagement
- Miles L , Hawkes R & French D (2023). Description of the nationally implemented National Health Service digital diabetes prevention programme and rationale for its development: mixed methods study. BMC Health Services Research
- Ravindrarajah R, Sutton M, Reeves D, Cotterill S, Mcmanus E, et al. (2023) Referral to the NHS Diabetes Prevention Programme and conversion from nondiabetic hyperglycaemia to type 2 diabetes mellitus in England: A matched cohort analysis. PLOS Medicine
- Ross J, Cotterill S, Bower P, Murray E. (2023) Influences on Patient Uptake of and Engagement With the National Health Service Digital Diabetes Prevention Programme: Qualitative Interview Study. Journal of Medical Internet Research
- Marsden A, Hann M, Barron E, Ross J, Valabhji J, Murray E, and Cotterill S. (2023). Comparison of weight change between face-to-face and digital delivery of the English National Health Service diabetes prevention programme: an exploratory non-inferiority study with imputation of plausible weight outcomes. Preventive Medicine Reports
- Hawkes R, Miles L, French D. (2023).What behaviour change technique content is offered to service users of the nationally implemented English NHS Digital Diabetes Prevention Programme: Analysis of multiple sources of intervention content. Preventive Medicine Reports
- Miles L, Hawkes R, French D. (2023). How the Behavior Change Content of a Nationally Implemented Digital Diabetes Prevention Program Is Understood and Used by Participants: Qualitative Study of Fidelity of Receipt and Enactment. Journal of Medical Internet Research
- Parkinson B, McManus E, Sutton M, Meacock R., (2022). Does recruiting patients to diabetes prevention programmes via primary care reinforce existing inequalities in care provision between general practices? A retrospective observational study. BMJ Quality and Safety
- McManus E, Meacock R, Parkinson B, Sutton M., (2022) Population level impact of the NHS Diabetes Prevention Programme on incidence of type 2 diabetes in England: An observational study. The Lancet Regional Health - Europe.
- Hawkes R.E, Miles L, Bower P, Cotterill S & French D.P., (2022) Assessing and ensuring fidelity of the nationally implemented English NHS diabetes prevention programme: lessons learned for the implementation of large-scale behaviour change programmes. Health Psychology and Behavioral Medicine.
- Blogs
- Experiences of attending an NHS bevaiour change programme and working with twp independently funded efalution teams - Eric Lwndes (Nov 2020)
- Test, Learn, Adapt - great ideas meet messy realities - Peter Bower & Sarah Cotterill (September 2019)
- ‘Doing exactly what it says on the tin’: how well is the NHS ‘Healthier You’ being delivered? - Elaine Cameron & David French (February 2019)
- Assessing the value of behaviour change ‘at scale’: the NHS Diabetes Prevention Programme - Peter Bower, Matt Sutton & Sarah Cotterill (July 2018)
- What is the Diabetes Prevention Programme and why is it important? - Carole Bennett (June 2018)
- How is the NHS Diabetes Prevention Programme being implemented? - Judith Gellatly (April 2019)
- Working at the Sharp End of an NHS Initiative: Making Sense of GP and Nurse Views on the NHS Diabetes Prevention Programme - Patrick Burch (March 2018)
- NHS Diabetes Prevention Programme – Fair and Equal Access - Sarah Cotterill (October 2017)
- Presentations
- DIPLOMA Webinar Slides - Peter Bower
- Learning lessons from implementation of a national diabetes prevention programme in England - Lisa Brunton
- 'Going the Distance' - An analysis of engagement and drop out among the first 100,000 referrals into the NHS Diabetes Prevention Programme - Sarah Cotterill
- The NHS Diabetes Prevention Programme delivery and patient experience: An observational study - Rhiannon Hawkes
- Challenges faced in Evaluating the National Health Services Diabetes Prevention Programme - Rathi Ravindrarajah
- Lay Summaries
Workpackage 1
 Download Qualitative Lay Summary
Download Qualitative Lay Summary Download Quantitative Lay Summary
Download Quantitative Lay SummaryWorkpackage 2
Workpackage 3
Workpackage 4
Workpackage 5
Workpackage 6
Workpackage 9
- Report
Visit the Policy@Manchester Planning for Prevention report for more information on:
More information

Co-Chief Investigator for DIPLOMA
Prof. Peter Bower